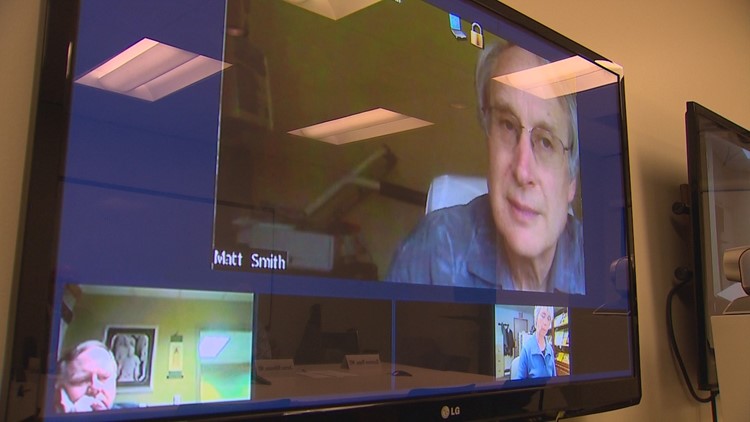
Each week, dozens of health care providers from rural Washington connect via video conference to a panel of specialists in Seattle with the hope of combating the opioid crisis statewide.
Dr. David Tauben, the Chief of the Division of Pain Medicine at UW, launched the “TelePain” program in 2011 to try and educate healthcare providers around the state about the new opioid prescription guidelines he helped to create years ago.
“Historically, opioid addiction was not a large problem in rural Washington, it's become that,” said Dr. Tauben of a nationwide trend.
However, rural communities often have far fewer resources to triage a complicated medical challenge that doesn’t have a simple solution.
“So many of our patients are dual diagnosis, where they have both an addiction problem and a psychiatric problem,” said Dr. Katherine Ottaway, a family care physician in Port Townsend.
Ottaway says her county currently has only one full-time psychiatrist, so she relies on the expertise from both psychiatry and pain management specialists on the TelePain calls. Doctors and healthcare providers from around the region can call in for advice in treating some of their most challenging cases.
“It’s been enormously helpful for all different reasons to have a panel of specialists who can give me multiple different ideas for how to work with the patients and also back up what my concerns are,” said Dr. Ottaway.
Since its launch, Dr. Tauben counts more than 500 consultations, across more than 300 locations. So far, it’s been funded by the state at a cost of $600,000 a year which includes follow-up with patients, according to UW. However, Dr. Tauben says he would like to see the program expanded nationwide, especially as lawmakers consider new opioid legislation in both the House and Senate.
“It’s translating into fewer deaths statewide, and it's also translating into a willingness by primary care doctors to take care of pain, in general, instead of saying ‘we don't take care of pain, go somewhere else; where are these people going to go?’”
“By educating the providers, by teaching them how to fish, not giving them the fish, they'll do great service to the state. It would be wonderful if we had continuing support at a national level, support for this model of “telehealth” which is provider-to-provider competency, training that’s based on real-life cases happening every day,” Tauben continued.