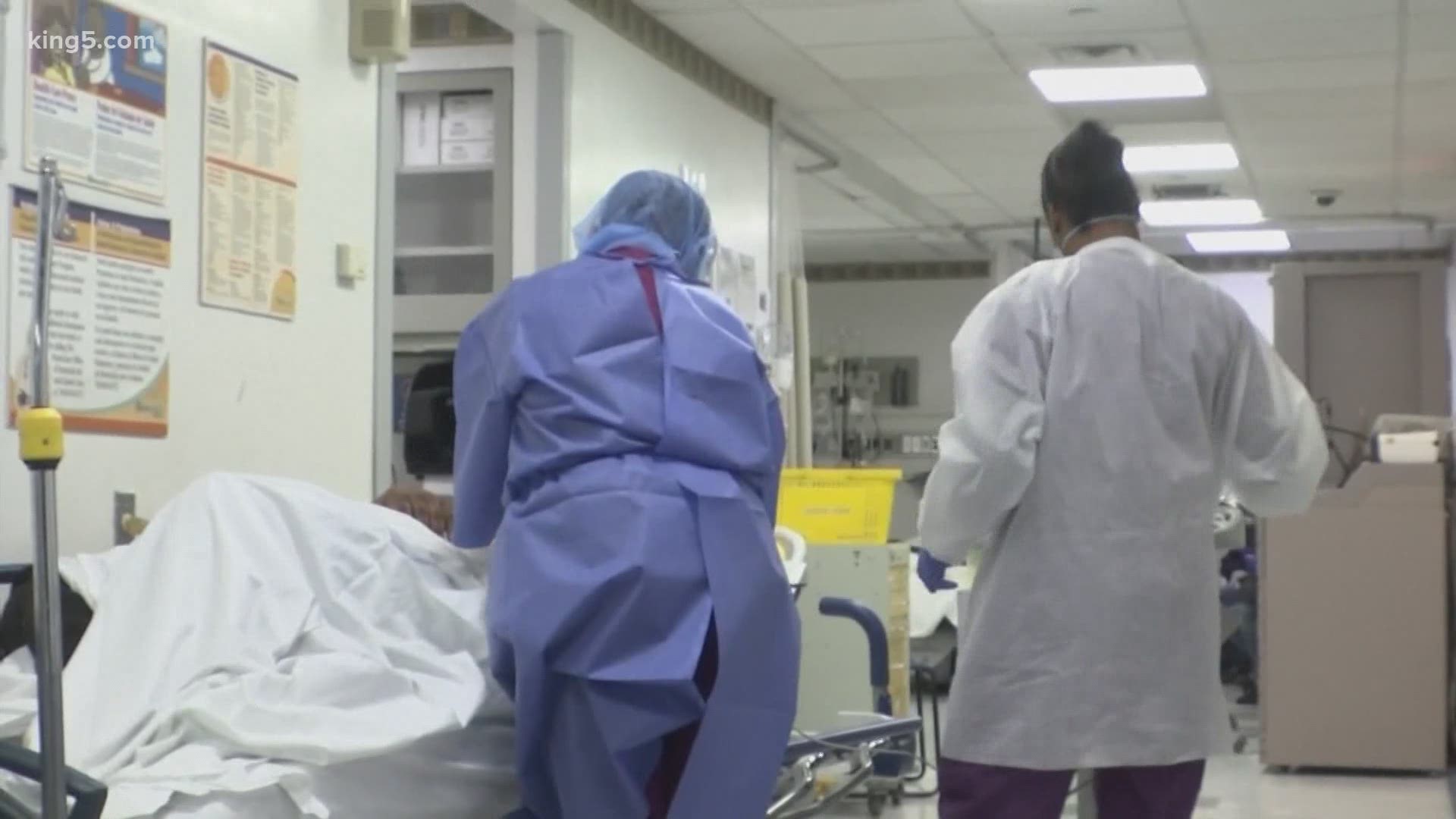
WASHINGTON — Two emergency room doctors and an emergency room nurse sat down at a virtual round table with KING 5 to talk about their experiences on the front lines of the pandemic and what they wish the public knew about their jobs.
Dr. Eric Shipley, Medical Director of the Emergency Department at Overlake Medical Center described the harrowing days after the first recorded COVID-19 death in the nation at nearby Life Care Center in Kirkland.
“It was pretty sobering. It was pretty overwhelming trying to understand that it was in our community, that it was not involving patients that had traveled,” said Shipley.
With the state of Washington at the epicenter of the pandemic, emergency rooms became ground zero.
“At one point, all of our ICU beds were filled in multiple hospitals with coronavirus patients,” said Dr. Karthik Swamy, Associate Emergency Room Medical Director at St. Clare Hospital
With the influx of patients, Dr. Shipley said there was uncertainty about whether healthcare staff were putting their own lives on the line.
“Those first two weeks at every hospital were very unnerving,” said Shipley. “You don’t know what you’re seeing. You’re not sure how to protect yourself. You’re not sure how to treat folks. If you are starting to feel like wow I might get infected in this, that’s when people start to feel vulnerable.”
Dr. Swamy said what the public may not know, is the grave reality of what it means to die of COVID-19, isolated and sometimes cut off from loved ones.
“I’ve had patients in the ICU who die alone because we can’t risk other people coming in there,” said Swamy. “I have to hold the phone up to their ear so their family members can talk to them. This is real.”
Data from the University of Washington’s Institute for Health Metrics and Evaluation (IHME) shows the number of COVID-19 deaths in Washington peaked at 26 per day in early April, then fell to 17 per day by May.
In Washington and across the country, stay at home orders have sparked backlash from protesters who doubt the severity of COVID-19 and the science behind it.
“It’s very frustrating,” said Tricia Jenkins, a registered nurse at Swedish Medical Center Center, Cherry Hill. “Lots of healthcare providers say, ‘Please stay at home so I can go to work,’” she said. “And that’s a real true statement. We need people to stay at home, keep this virus at bay.”
The latest projections from the IMHE show that as states ease social distancing measures, the number of deaths nationwide could climb to 135,000. Karthik said he supports a slow, phased reopening of Washington, but if that doesn’t happen, winter could bring a deadly second wave of COVID-19.
“What is pretty much guaranteed is when a lot of the quarantine measures are moved, we will see another spike,” said Swamy. But he said if reopening is progressive, that spike could be manageable.
“Which is why it’s very, very important that you can’t just go outside and return to your life like it was three months ago. That will end very poorly. I’ll tell you that right now,” said Swamy.
Shipley said one scenario is that the number of COVID-19 cases could rise in December, January and February, just as flu season is in full swing.
“We have to be able to surge if we get another spike particularly later in the year,” said Shipley. “We’re much better prepared now than we were.”
Jenkins and Swamy said large-scale testing is needed to create models to track the spread of COVID-19 more accurately.
“That’s going to give us so much information, especially when it comes time to reopen the economy,” said Swamy.”
“I don’t think that we’ll really be able to move forward in a full phase of opening our communities until we do have the capacity to test people, trace who they’ve been with, and also have some treatment processes for people who are sick with coronavirus,” said Jenkins.
All of the healthcare workers were in agreement about what they will remember most about this moment in history: the courage of their colleagues.
“The thing the general public does not see is really the heroics of the staff,” said Shipley. “I see young nurses with children that are three and five [years-old], and they’re going into rooms with their spacesuits and they’re not thinking about themselves.”
“There are a lot of personal sacrifices that people in healthcare are making right now,” said Jenkins. “I have my children live with my mom when I work my straight shift and I wait two days to make sure I don’t have symptoms before I pick them up.”
Jenkins said another hidden aspect of this pandemic is the effect of the pandemic on the mental health of hospital employees.
“There has been a lot of trauma on healthcare workers,” she said. “There’s going to need to be a lot of repair work done for healthcare professionals and their well-being after this is over.”